At Sírio-Libanês Hospital in São Paulo, Brazil, patients are now starting radiation treatment on average two days sooner. Reducing the time from simulation to the first day of treatment is just one of the many benefits that the Sírio-Libanês hospitals in São Paulo and Brasilia have gained from the ARIA® oncology information system (OIS) after engaging one of Varian’s clinical consulting services teams to help them optimize their use of ARIA.
The Sírio-Libanês hospitals provide comprehensive cancer care, including the full range of radiotherapy techniques. Combined, the two hospitals treat about 140 patients per day with some form of external beam radiotherapy, including 3D Conformal, IMRT, SBRT, SRT, and SRS.
Formerly, the main hospital in São Paulo and its satellite hospital in Brasilia didn’t have reliable data on how long patients were waiting from simulation to the start of treatment. Now they have the data, captured by ARIA, for this and many other metrics. This is allowing them to continuously improve workflow processes for ever greater efficiency and consistency.
Recognizing the potential for the ARIA OIS to be much more than a simple record-and-verify tool, the Sírio-Libanês team engaged Varian’s global clinical operations consultants to help them understand the system’s full capabilities as well as how to leverage them to organize and manage workflow. The collaboration with Varian started at the satellite hospital in Brasilia, which became the proving ground for improvements that were later extended to São Paulo. Varian consultants Hana Tobe and Ana Maria Bonfiglioli Lage were assigned to the task.
The path to consistency
While getting new patients started on their treatment sooner was an important goal, an even higher priority was to be more consistent, says Jose Eduardo Vaz Nascimento, chief physicist at Sírio-Libanês Hospital--Brasilia. “Average or mean wait time did not concern us as much as the variability we were experiencing.” Often the inconsistency in wait times was precipitated by urgent cases, requiring dosimetrists and physicists to interrupt their work for the higher priority. These urgent cases make up approximately 15 percent of Sírio-Libanês patients. The clinical team wanted to narrow the deviation from the mean wait time and assure that no task fell through the cracks or caused unnecessary delay.
“Understanding the department’s processes in detail as well as the needs of each team was critical,” says Ana Maria Bonfiglioli Lage, clinical application specialist, one of two Varian consultants assigned to the Sírio-Libanês project. “That was fundamental to our ability to help them develop an efficient workflow that could be supported by the features of the ARIA system. Every department has a routine and often, inefficient protocols are being followed unnoticed. It is our job to analyze the workflow and suggest simpler processes. We spent a full day—ninety minutes each with a nurse, a physicist, a doctor, a technician, a dosimetrist, a nursing assistant, and a receptionist, to really understand how all the functions were working together. That way, we could identify ways that ARIA could streamline the process.”
 The medical physics team at Sírio-Libanês. Seated: Cecília Maria Kalil Haddad, Pedro Augusto Minorin Mendes Ramos. Standing: Edilson Lopes Pelosi, Wellington Furtado Pimento Neves Junior, Anselmo Mancini
The medical physics team at Sírio-Libanês. Seated: Cecília Maria Kalil Haddad, Pedro Augusto Minorin Mendes Ramos. Standing: Edilson Lopes Pelosi, Wellington Furtado Pimento Neves Junior, Anselmo Mancini
“We reviewed and observed many important processes with the clinical team, including referral/front desk, consultation visit, weekly on-treatment visit, follow-up visit, initial simulation, treatment planning, daily treatment, final treatment, charge capture, and physics weekly chart check,” adds Hana Tobe, the global clinical operations consultant who worked with Ana Maria on the project. “After our initial visit, we produced a report of our findings and the opportunities for improved clinical and business processes. During a second visit, we demonstrated how ARIA functionality could be harnessed to improve processes. We then worked with the customer to configure ARIA accordingly. Select team members were trained on the newly implemented workflows.”
For example: Ana Maria and Hana helped the department deploy tasked-based CarePaths within the ARIA system. In consultation with the Brasilia team, they recommended a set of CarePaths that would automate and regulate the progress of all cases through simulation, planning, treatment, and follow up. Every patient is now assigned to the General Carepath or the Urgent Carepath, as determined by the physician.
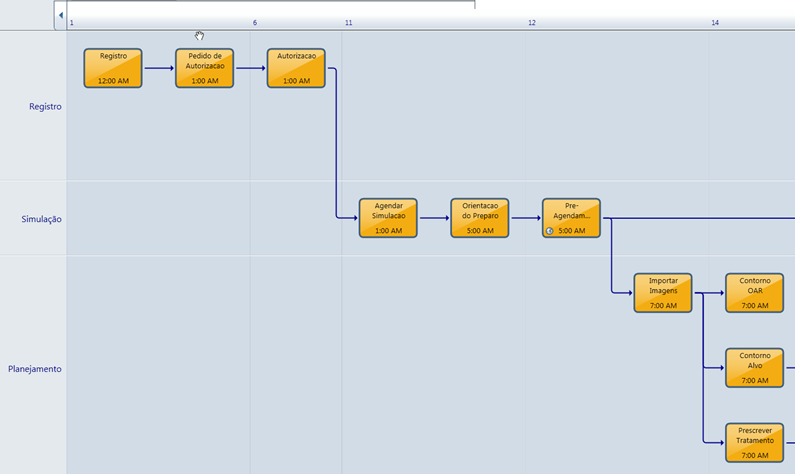
Details from an ARIA CarePath
In addition, the Varian consultants recommended adoption of a set of QA Carepaths specific to the different treatment techniques prescribed—3D conformal, IMRT, SBRT, and so on. “By implementing Carepaths, we now follow a set pattern and have greater consistency in workflow. We know at a glance the next step for every patient,” says Eduardo. Setting up the Carepaths initially proved quick and easy, as was making changes as the team gained experience, reports Eduardo. “We spent most of the time discussing the best workflow among the team. The Varian consultants facilitated that discussion,” he adds.
With the implementation of Carepaths, treatment planning now takes less time. Cecília Maria Kalil Haddad, chief physicist at the São Paulo hospital, reports that, in the first six months of using ARIA, the average planning time span decreased from seven days to five days. “Five days may seem like a long time in some clinics, but São Paulo is a teaching hospital. We train 10 resident radiation oncologists and physicists per year, so our workflow builds in additional time and tasks for training and reviews by senior staff,” she explains. “The process is now smoother and the handoffs more consistent.”
Communications transformed
While automating and streamlining workflow to ensure consistency, optimal use of ARIA has also transformed team communications. Formerly, radiation oncologists who needed to prioritize an urgent case would pick up the telephone to the dosimetrist or walk down the hall to find the medical physicist. Dosimetrists would leave paper notes in the chart about the status of plans. Physicists would send text messages to physicians about plan reviews. Communication among all the members of the care team—from the front desk to the RNs--was mostly manual and one-to-one.
However, that’s no longer the case. From simulation to patient discharge and follow-up, all workflow tasks and intra-team communications are managed by ARIA. “Everyone with permissions can access the ARIA system to look up the up-to-the-minute status of every patient, plan, task, and treatment,” says Pedro Mendes Ramos, physicist at Sírio-Libanês Hospital in São Paulo. “And everyone can see what they need to do next. Tasks are ‘pushed’ to the right person at the right time by the system; staff members no longer need to call each other or physically find one another in the department to trigger a next step. Communication has become more integrated and seamless.”
One way that communication has been improved is with the use of the Documents and Encounters features in ARIA. Documents are linked between tasks and available in Encounters. Pedro illustrates the functionality: “On the first visit, the radiation oncologist enters his or her expectations for Simulation in a template document, which is then available in the Simulation Encounter. At the time of Simulation, therapists used to document the procedure by making narrative notes on a blank sheet of paper. Now they choose a template in ARIA with a clickable checklist and fillable boxes, which is then available to the radiation therapists at the time of treatment. The templates make communication clearer and more consistent, which saves time while enhancing safety. Pedro figures that they are saving between 10 and 20 minutes per patient by having all the documents available online, instead of having to locate paper files. And time saved translates to more capacity to treat patients. “At this point we are ‘paper light,’ in the process to becoming paperless, which is our goal for this year,” says Pedro.
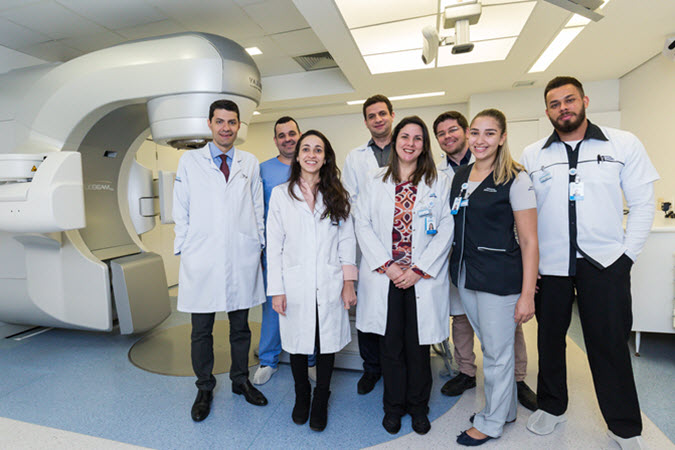 The clinical team: Dr. Rafael Gadia, department director; Alex Xavier, lead therapist; Isabela Gondim, physicist; José Eduardo Nascimento, chief physicist; Tatiana Calil, dosimetrist; João Paulo Leite, physicist; Larissa Felix, nurse; Bruno Emanuel Santos, nurse technician
The clinical team: Dr. Rafael Gadia, department director; Alex Xavier, lead therapist; Isabela Gondim, physicist; José Eduardo Nascimento, chief physicist; Tatiana Calil, dosimetrist; João Paulo Leite, physicist; Larissa Felix, nurse; Bruno Emanuel Santos, nurse technician
Better control through data
As Cecília and Eduardo see it, however, the main benefit of going digital through ARIA is the improved access to data for process improvement and decision-making. “Time saved is not the greatest improvement we have gained from ARIA. The greatest improvement is organization, so we can control time better. Now we have the data to see how we use our time and learn how we can use it better,” says Eduardo.
The Sírio-Libanês teams are now able to create reports and get more data out of ARIA to answer key questions, understand trends, and support decisions. “We have been able to build ARIA reports to answer key questions. There are 15 to 20 indicators that we track,” says Cecília. These include metrics about machine capacity compared to utilization; average treatment time for specific disease sites (H&N, prostate, breast, and so on); the time span from simulation to first day of treatment; and the difference between the scheduled start time and the actual start time of treatment sessions. The data ARIA captures enable the hospitals to understand their capacity for new patients or to justify the addition of new systems or techniques, or to make slight changes to processes that add to efficiency. “I knew that ARIA could provide answers to these and more questions, but I wasn’t certain about how to mine that data or the time involved. The consulting was very helpful,” says Eduardo.
“We didn’t realize the full potential ARIA, so I don’t know if we would be where we are now without the consulting. Hana and Ana Maria showed us how to use the system to continually improve workflow and we have been able to share that knowledge with the staff in São Paulo. Both staffs have embraced ARIA whole-heartedly,” Eduardo concludes.