In 2015, the Radiation Oncology Department of Loyola University Medical Center transitioned to the ARIA® oncology information system. Today, the department efficiently runs its daily clinical operations on ARIA. “We manage the whole department through ARIA Care Paths. This enables us to see, at any given time, where every patient is in the treatment process. We can also see the workload for every group and staff member. We can see the whole picture,” said John Roeske, professor and director of medical physics at Loyola. Seeing the whole picture is essential in a department that treats more than a thousand patients a year, with every form of radiation therapy, including EBRT, HDR and LDR brachytherapy, SRS, intraoperative radiotherapy, and proton therapy through partners.
In ARIA, Care Paths can be created for a variety of clinical, operational or financial workflows. Based on the 6-Sigma methodology for improving processes, Care Paths capture workflows, ensure that tasks are completed, and auto-escalate overdue tasks for completion. This article highlights two of the ways that team members at Loyola Radiation Oncology are using ARIA Care Paths to improve processes and meet their goals for quality care. One is to transition to a prospective peer review process that reviews contours before the start of treatment. The other is to improve coordination with Medical Oncology.
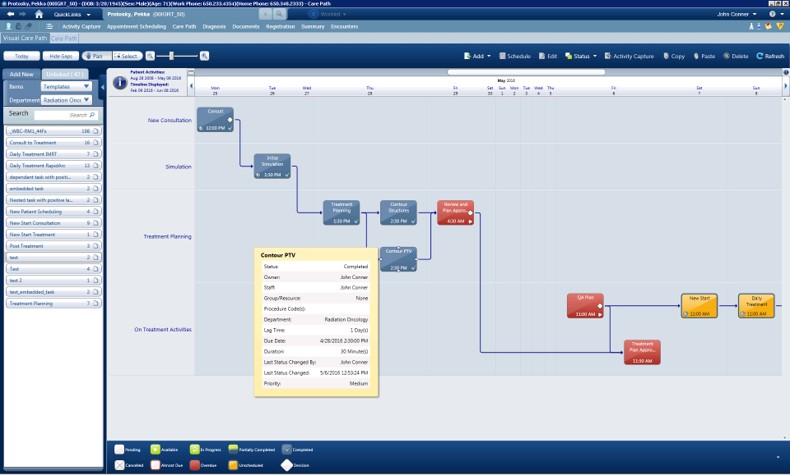 Care Paths capture workflows, ensure tasks are completed, and auto-escalate overdue tasks for completion.
Care Paths capture workflows, ensure tasks are completed, and auto-escalate overdue tasks for completion.
Prospective contouring and planning rounds
Previously, Loyola’s peer review program consisted of weekly chart rounds performed in the first week of the patient’s treatment. “While most centers conduct peer review through weekly retrospective “chart rounds,” there is ostensibly greater benefit in completing chart rounds in a prospective, daily format,” said Murat Surucu, PhD, associate professor and chief of clinical physics.
In October 2015, the team implemented daily contouring and planning rounds using ARIA Care Paths. At the time of CT simulation, patients are assigned to one of five Care Paths based on urgency and complexity (Standard, Urgent, Palliative Non-Emergent, Emergent, and Special Procedures). Specific tasks are implemented based on the group and Care Path to which the patient has been assigned.
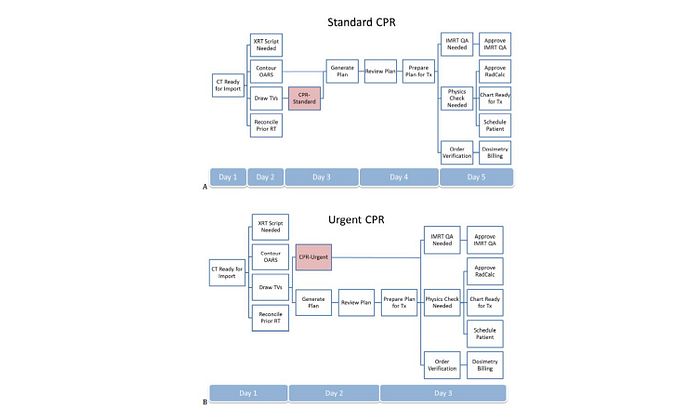
For example, In the Standard Care Path, contours are reviewed before the start of planning as part of a “Contour Plan Review” (CPR) task. This CPR task becomes available in the Care Path after the physician completes drawing the tumor volume. The next step—the “Generate Plan” task—does not become available for dosimetrists until the case has been presented at Contour Plan Review (CPR) rounds. In the Urgent Care Path, the “CPR-Urgent” task becomes available after the tumor volume has been drawn, while the “Generate Plan” task permits planning simultaneously.
Of the 4,759 cases reviewed under the new CPR program by the end of May 29, 2018, 125 required major contour and plan changes and repeat presentation. Another 102 were recommended for minor modification. “Contouring and planning rounds were successfully implemented in our clinic using the tools provided within ARIA,” reported Surucu. “The CPR method has made our peer review more thorough and improved standardization.” More information about the CPR method can be found in a paper that the Loyola team recently published in Advances in Radiation Oncology (2019).1
Improved coordination with Medical Oncology
Loyola also recently implemented a Care Path to coordinate with the medical oncology team to avoid delayed starts of concomitant chemotherapy.
Loyola clinicians prefer to schedule patients for radiation treatment delivery after the radiotherapy plan is complete. In this way, no patient ever shows up for treatment to find that the plan isn’t ready. However, the addition of chemotherapy to the mix provides another layer of complexity in coordination. Coordinating with Medical Oncology takes a couple of days to ensure they have the necessary chairs, staff, and medication available.
“We want to start the patients on treatment as soon as possible for better care. We expect that by starting discussions with the medical oncology group sooner, we will save time, perhaps a few days,” said Surucu. For that reason, Radiation Oncology created a Care Path for multi-modality patients. When a radiotherapy plan is approved, a task is triggered for schedulers to start coordinating chemotherapy. The results aren’t yet in, but the coordination is more structured, automated, and measurable.
These are two ways that the Loyola Radiation Oncology Department is applying its oncology information system, ARIA, to continuously improve the efficiency of its care delivery. However, Loyola is looking well beyond these clinical and operational efficiencies. “My interest is machine learning and artificial intelligence,” Roeske concluded. “I think ARIA is potentially an area where we can be extracting data to train models in new paradigms that will impact future patient care. That's a future direction that I would like to see.”
Varian and Roeske are on the same page, when it comes to enthusiasm about the potential for machine learning and artificial intelligence.
“Varian is pursuing numerous ways of using machine learning (ML) and artificial intelligence (AI) in our technology development efforts, from contouring tools and RapidPlan® functionality in Eclipse™ treatment planning to the clinical decision support tools we’re building into the 360 Oncology™ care management platform,” says Corey Zankowski, senior vice president, Varian Oncology Software Solutions. “Ultimately I think ML and AI will give us both efficiency and quality improvements. In the longer term, we’ll see significant automation of routine tasks that liberate clinical professionals to focus on the important patient-care activities that machines cannot offer.”
1Surucu M, Bajaj A, Roeske JC, Block AM, Price J, Small W Jr., Solanki AA. The Impact of Transitioning to Prospective Contouring and Planning Rounds as Peer Review, Advances in Radiation Oncology (2019), doi: https://doi.org/10.1016/j.adro.2019.03.004.
The information captured herein represents the genuine experience of the attributed individuals and may not necessarily represent the views of Varian or the above referenced institutions. Individuals were not compensated for their participation.