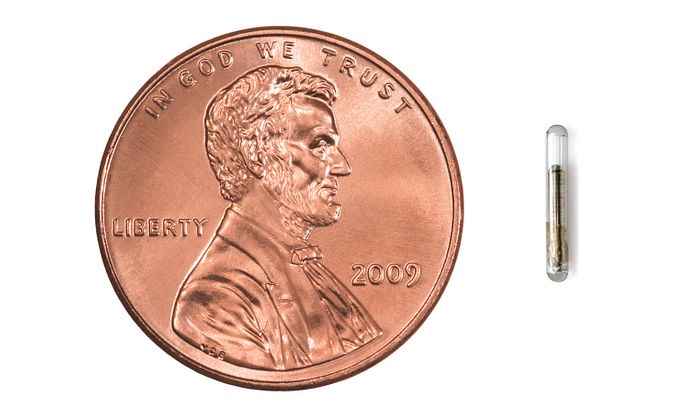For patients presenting with liver cancer at Aarhus University Hospital in Denmark, intrafraction motion had always been a serious impediment to SBRT treatment. Due to respiration, the liver is prone to movement. It can shift as much as three centimeters during SBRT, according to Esben Worm, Ph.D., a medical physicist at Aarhus. Target drift is also a concern. “We see baseline shifts or drifts of up to one centimeter during a single treatment,” says Worm. In the face of these uncertainties, clinicians historically had few options other than to increase margins. But doing so potentially exposed critical structures near the tumor—spinal cord, esophagus, duodenum, intestines, kidneys—to radiation.
Recently, Aarhus clinicians studied and reported on the use of Calypso® Soft Tissue Beacon® transponders to track liver tumor position and motion during SBRT treatments.1
In an outpatient procedure taking about 20 minutes, three Calypso transponders are implanted around the tumor, transmitting its location at a rate of 25 Hz. The Calypso system locks onto the signal during patient setup and tracks it continuously throughout the treatment. “We use the 17G Beacon transponder with 50 percent smaller cross-sectional area than the 14G version,” says Lars Peter Larsen, M.D., of the Aarhus department of radiology. The choice is logical: A smaller needle gauge is always preferable for a percutaneous implant in tissue surrounding the liver. “While we have seen no complications from either transponder, we know from studies that the risk of bleeding is lower with the thinner needle,” Dr. Larsen says.
During simulation, clinicians take a 4D CT scan and an exhale breath-hold CT scan with contrast. “An advantage of using the Calypso system is that we can plan the treatment on the exhale scan, which usually is of good quality,” says Dr. Worm.
The transponders are defined along with the target and structure contouring, and then transferred to the Calypso system. The SBRT plans at Aarhus University Hospital usually consist of a minimum of seven fields. “In planning the fields, some care is involved to consider gantry angles and couch motion to avoid collisions with the Calypso cart,” says Per Poulsen, Ph.D., professor at the Aarhus Institute of Clinical Medicine.
Calypso real-time tracking is so accurate that Aarhus University Hospital is now using it for gated liver treatments, a highly advanced application of the technology. “We had not done respiratory gating for liver SBRT until the Calypso system enabled us to track internal motion,” says Dr. Poulsen. “Now we can follow the motion of what’s going on inside the patients without adding imaging radiation dose.” The result, he says, is that clinicians can now see intrafraction baseline drifts that were not previously visible. “During the course of the treatment, we can observe the drifts, pause the system, and correct for them by making couch adjustments."
With the capability for real-time tracking and gated treatment, the Aarhus team has been able to reduce margins to 7 mm from the 10 mm typical of non-gated treatments. But regardless of treatment type or margin size, Calypso means that clinicians can compensate for respiratory motion and drift and hit the target with greater accuracy. “We believe real-time tracking with the Calypso system reduces the chance of side effects and may ultimately enable us to increase the dose for improved outcomes,” says Morten Hoyer, M.D., professor at Aarhus University Hospital.
1Worm ES, Hoyer M, Hansen R et al. A Prospective Cohort Study of Gated Stereotactic Liver Radiation Therapy Using Continuous Internal Electromagnetic Motion Monitoring. Int J Radiation Oncol Biol Phys, Vol. 101, No. 2, pp. 366-375, 2018
_______________________________________________________
The information captured herein represents the genuine experience of the attributed individuals and may not necessarily represent the views of Varian or the above referenced institution. Individuals were not compensated for their participation. Radiation treatment may not be appropriate for all cancers. Individual results may vary.