Expansion of Brachytherapy Suite Opens Door for More Treatments
Varian’s Bravos™ afterloader system was designed to streamline the overall high-dose-rate (HDR) brachytherapy treatment process, from planning to delivery. Brachytherapy treats cancer by placing radioactive sources directly into or next to the area requiring treatment. Bravos integrates with the BrachyVision™ treatment planning system to create plans that deliver a high dose to the targeted area with minimal impact on surrounding healthy tissues.
Varian introduced the Bravos afterloader system at ASTRO in 2018, in response to a growing need for an easy-to-use, efficient system. Intuitive, smart features, such as a customizable pre-treatment checklist and a color-coded LED display to confirm applicator connections, are designed to improve efficiency and safety, freeing clinicians to focus more on their patients, rather than their treatment tools.
In this article, the clinical team at the UK-based Norfolk and Norwich University Hospital (NNUH) shares its experiences as the first site to use the new Bravos system.
Expanding beyond gynecological cancer
The Bravos system was installed at NNUH in 2018 as part of a new, specially built brachytherapy treatment suite that also included a multi-purpose room for anesthesia and treatment, and a dedicated recovery area.
Prior to November 2018, NNUH was using brachytherapy only to treat gynecological cancers. However, brachytherapy is well established as a treatment for localized prostate cancer. HDR brachytherapy offers a means to deliver hypo-fractionated dose escalation within the limits of normal tissue tolerances, helping to reduce the risk to healthy organs and improve disease control.1 Furthermore, recent studies indicate that adding HDR brachytherapy to a course of external beam radiotherapy (EBRT) can improve biochemical and survival outcomes.2
The new brachytherapy suite, with its Bravos HDR system, enables NNUH to keep up with these kinds of advanced therapies that help improve outcomes and serve an aging demographic within their community.
“The addition of Bravos has allowed us to start treating prostate patients with brachytherapy, as well as streamline the process for the gynecological patients we were already treating,” explains Sam Worster, advanced practitioner of prostate brachytherapy at NNUH. “Everything about the system is designed to help speed up treatments and improve patient safety—from the intuitive touchscreen to the machine’s easy maneuverability around the operating room to the built-in checklists. It’s a massive step forward.”
As an advanced practitioner and radiographer, Worster’s role is to review potential brachytherapy patients with the medical team, and then take them through the procedure from start to finish. He plans each patient’s treatment alongside the doctors, reviews it with the physicist, delivers the treatment, and then follows up directly to help manage any side effects and ensure patients receive a continuum of care.
“We typically treat patients on an out-patient basis in one day, so it’s important that the entire process is as efficient and seamless as possible,” he says. “Treatment with the Bravos technology can take anywhere from 20 to 40 minutes, depending on how many channels we use.”
This efficiency means that Worster gets to spend more time with his patients. “I’m lucky that my role allows me to spend a lot of time with patients, helping them through their diagnosis and their treatment journey,” he says. “The Bravos system completely supports this mission.”
Integrating treatment planning and delivery
 Vicki Currie is the lead clinical scientist for brachytherapy in the NNUH Radiotherapy Physics department and leads the commissioning of Bravos and brachytherapy treatment planning, including set up, testing, and afterloader verification.
Vicki Currie is the lead clinical scientist for brachytherapy in the NNUH Radiotherapy Physics department and leads the commissioning of Bravos and brachytherapy treatment planning, including set up, testing, and afterloader verification.
“We’re part of a multidisciplinary team that delivers treatments, ensures radiation protection is in place, transfers plans to the machine, and verifies that the dose is delivered safely and accurately,” she says. “Bravos has helped streamline the entire process as it fully integrates with treatment planning. The Bravos system also runs its own length check, so we can see what length it measures and verify it matches the plan. It even tells us whether the path is clear for the source.”
Not only does the length-check feature on Bravos provide an extra safety check, but it also takes place while clinicians are still in the room with the patient.
“Previously, we had to carry out length checks after we’d left the room and if there was an issue, we had to go back in. This can cause anxiety for the patients,” Currie explains. “Now, if there’s any variance in length or a blockage, Bravos lets us know and we can correct it before leaving the room, without causing anxiety for the patient.”
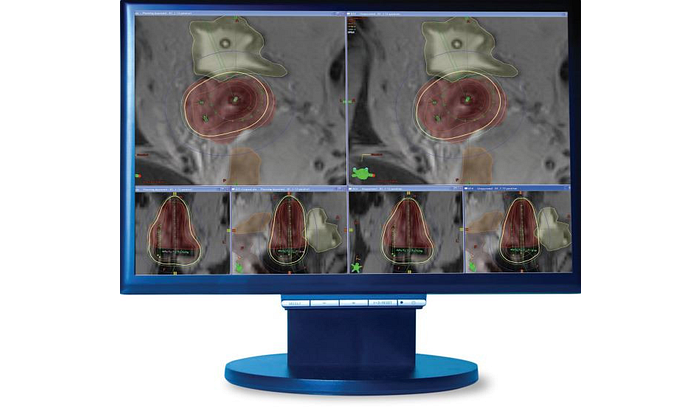
The integration of treatment planning and delivery is also a huge plus for Katie Cooper, consultant radiographer for brachytherapy, who oversees brachytherapy treatments at NNUH. The brachytherapy suite uses BrachyVision with Eclipse™ treatment planning to deliver treatments.
“As we look at streamlining our workflows, the built-in software means we can reduce the use of treatment spreadsheets and further improve the efficiency of paperless processes within the department,” Cooper explains. “Not only can we customize the brachytherapy checklist to include everything we need to make treatment safer, but there is also the potential to develop the way in which we record patient’s treatments. The inclusion of electronic signatures ensures compliance with the Ionizing Radiation (Medical Exposure) Regulations (IR(ME)R).
NNUH uses both external beam radiotherapy and HDR brachytherapy to treat prostate and gynecological tumors. Most gynecological treatments involve external beam radiotherapy first, followed by brachytherapy, while prostate treatments start with brachytherapy.
Brachytherapy has been shown to increase patient survival rates in some cases, when combined with external beam radiotherapy. According to one study, adding brachytherapy to external beam radiotherapy for cervical cancer showed a 12.8% increased survival rate at four years.3
“Developing the brachytherapy treatment suite was a joint effort with Varian,” she says. “The training was excellent, clear and in depth, and Varian has been very supportive in getting us off the ground and going. As more people are trained and the prostate service grows, we’re also looking at expanding to treat cancers of the esophagus, rectum, and skin. We’re optimistic that this will make a huge difference to patients in the area.”
1 Hoskin PJ et al. Randomized trial of external beam radiotherapy alone or combined with high-dose-rate brachytherapy boost for localized prostate cancer. Radiother Oncol. 2012 May;103(2):217-22. doi: 10.1016/j.radonc.2012.01.007.
2 Wedde TB et al. Ten-year survival after High-Dose-Rate Brachytherapy combined with External Beam Radiation Therapy in high-risk prostate cancer: A comparison with the Norwegian SPCG-7 cohort. Radiother Oncol. 2019 Mar;132:211-217. doi: 10.1016/j.radonc.2018.10.013. Epub 2018 Oct 30.
3 Han K et al. Trends in the utilization of brachytherapy in cervical cancer in the United States. Int J Radiat Oncol Biol Phys, 2013; 87:111-119.
The information captured herein represents the genuine experience of the attributed individuals and may not necessarily represent the views of Varian or the above referenced institutions. Individuals were not compensated for their participation. Individual results may vary.